Lymphedema is a chronic and progressive condition caused by lymphatic system dysfunction that results in the accumulation of protein-rich fluid within the interstitial tissues. Early recognition and referral are essential to prevent long-term complications such as fibrosis, chronic inflammation, and recurrent cellulitis. Clinicians across many specialties—including oncology, primary care, vascular medicine, orthopedics, and rehabilitation—may be the first to observe early signs of the condition. Understanding how to identify lymphedema and when to refer patients to a certified lymphedema therapist allows for earlier intervention, improved outcomes through conservative and evidence-based management, and better long-term management of this progressive condition.
Key Takeaways
- Early detection is critical: Mild swelling, heaviness, or tightness may be the first signs of lymphedema.
- Look for characteristic physical findings: pitting edema, asymmetry between limbs, skin changes, and reduced tissue elasticity.
- Patients with cancer treatment history are at higher risk, especially after lymph node removal or radiation therapy.
- Prompt referral to a Certified Lymphedema Therapist (CLT) allows early treatment using Complete Decongestive Therapy (CDT).
- Clinicians play a vital role in screening, especially in patients with persistent or unexplained swelling.
Table of Contents
Understanding Lymphedema
The lymphatic system plays a critical role in maintaining fluid balance, immune function, and waste removal from tissues. When lymphatic vessels or nodes are damaged or impaired, lymph fluid accumulates in the interstitial space, leading to the swelling known as lymphedema.
Lymphedema can be classified into two categories:
Primary Lymphedema
- Caused by congenital abnormalities of the lymphatic system
- May appear at birth, during puberty, or later in adulthood
Secondary Lymphedema
- Caused by damage to lymphatic structures
- Common causes include:
- Cancer surgery involving lymph node removal
- Radiation therapy
- Trauma or infection
- Chronic venous insufficiency
- Obesity
Secondary lymphedema is most commonly seen following breast cancer, gynecologic cancer, prostate cancer, and melanoma treatment, though it can occur after many types of medical interventions.
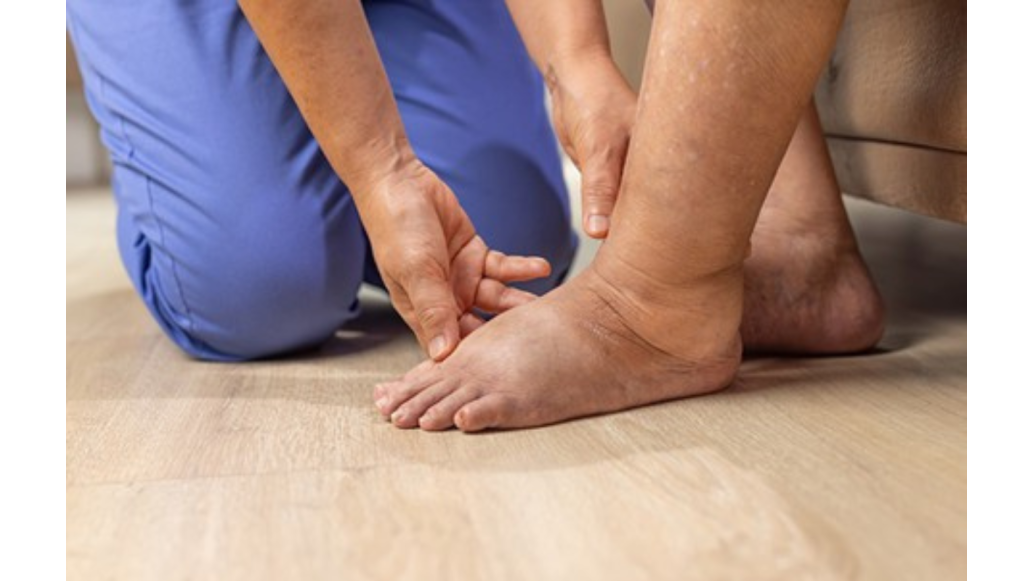
Early Signs Clinicians Should Look For
Lymphedema often develops gradually. Early symptoms may be subtle and easily mistaken for normal swelling or edema.
Clinicians should consider lymphedema when patients report:
Persistent Swelling
Swelling that does not resolve overnight or with elevation may indicate lymphatic dysfunction.
Heaviness or Fullness in the Limb
Patients often describe the affected area as heavy, tight, or fatigued, even before noticeable swelling develops.
Tightness of Skin or Clothing
Early lymphatic congestion can cause rings, watches, or clothing to feel tighter.
Decreased Flexibility
Swelling may limit joint mobility, particularly in the fingers, wrist, ankle, or knee.
Mild Skin Changes
Patients may experience:
- Skin thickening
- Reduced skin elasticity
- A sensation of skin tightness
Recognizing these early symptoms allows clinicians to intervene before irreversible tissue changes occur.
Physical Examination Findings
A careful physical examination can reveal several hallmark signs of lymphedema.
Limb Asymmetry
Comparing the affected limb to the unaffected limb may reveal visible size differences. Even small changes in circumference can indicate early disease.
Pitting Edema
In early lymphedema, applying gentle pressure to the skin may leave a temporary indentation.
Stemmer Sign
A positive Stemmer sign occurs when the clinician cannot pinch the skin at the base of the second toe or finger due to skin thickening. This is a strong indicator of lymphedema.
Skin Changes
As the condition progresses, clinicians may observe:
- Hyperkeratosis
- Fibrosis
- Skin thickening
- Papillomatosis
Recurrent Cellulitis
Frequent skin infections in the same limb can be a sign of impaired lymphatic drainage.
Patients at Higher Risk for Lymphedema
Certain populations have a significantly increased risk of developing lymphedema. Screening these patients is especially important.
Cancer Survivors
Patients with a history of:
- Lymph node dissection
- Sentinel lymph node biopsy
- Radiation therapy
are at increased risk of developing lymphedema months or even years after treatment.
Surgical Patients
Procedures that disrupt lymphatic vessels may increase risk, including:
- Orthopedic surgeries
- Vascular surgeries
- Cosmetic procedures involving lymphatic structures
Chronic Venous Disease
Long-standing venous insufficiency can overwhelm lymphatic drainage, leading to phlebolymphedema.
Obesity
Higher body mass index increases pressure on lymphatic vessels and impairs lymphatic flow.
Trauma or Infection
Injury to the lymphatic system or repeated infections may also trigger lymphedema.
When to Refer to a Certified Lymphedema Therapist
Clinicians should consider referral when any of the following are present:
Persistent Limb Swelling
Swelling lasting longer than three months without another clear cause should prompt evaluation.
Post-Cancer Treatment Swelling
Any swelling following lymph node removal or radiation therapy should be evaluated by a CLT.
Recurrent Cellulitis
Frequent infections may indicate impaired lymphatic drainage.
Functional Limitations
If swelling interferes with mobility, daily activities, or range of motion, early intervention is essential.
Abnormal Limb Measurements
Even small differences in limb circumference can signal early lymphedema.
Early referral allows patients to receive treatment before the condition progresses to fibrosis and chronic tissue changes.
Role of Lymphedema Therapy
Certified Lymphedema Therapists treat patients using Complete Decongestive Therapy (CDT), the gold standard for lymphedema management.
CDT includes:
Manual Lymphatic Drainage
A gentle massage technique that stimulates lymphatic flow.
Compression Therapy
Short-stretch bandaging and compression garments help maintain fluid reduction.
Therapeutic Exercise
Movement enhances lymph circulation and supports fluid drainage.
Skin and Nail Care
Proper care helps prevent infections and protects fragile tissue.
Early treatment allows patients to manage symptoms effectively and maintain quality of life.
Popular Lymphedema Products
Medical Disclaimer: The information provided on this site, including text, graphics, images, and other material are for informational purposes only and are not intended to substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other healthcare professional with any questions or concerns you may have regarding your condition.








 France
France Australia
Australia