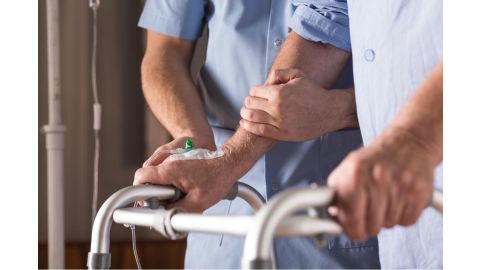
Fall prevention should be a multi-disciplinary effort including physicians, physical and occupational therapists, patients and their families, and of course, nurses.
Because RNs and LPNs spend so much time with patients, a lot of the responsibility falls on you during direct care. Are you doing everything possible to prevent your patients from falling?
Table of Contents
How often do patients fall?
How many patient falls result in injuries?
How does your unit define and record falls?
The Role of Nurses in Fall Prevention Programs
Follow The Nursing Process for Falls
Patient Fall Risk Factors
Universal Fall Precautions
Patient-Specific Fall Prevention Strategies
Protect Your Patients from Injuries if a Fall Occurs
Learn More About Fall Prevention
How often do patients fall?
700,000 to 1 million hospitalized patients fall every year according to estimates by the Agency for Healthcare Research and Quality.1 Elderly patients are at an increased risk for falls. In one study on long term care residents, 56.2% of their 395 resident sample fell at least once over the six month study.2 The study concluded that falls are common among LTC residents and remain an important problem.
Fall rates vary across units due to a variety of factors. One study from the National Database of Nursing Quality Indicators found fall rates of:3
- Intensive Care Unit: 1.30 falls/1,000 patient days
- Surgical: 2.79 falls/1,000 patient days
- Stepdown: 3.44 falls/1,000 patient days
- Medical-Surgical: 3.92 falls/1,000 patient days
- Medical: 4.54 falls/1,000 patient days
- Rehabilitation: 7.15 falls/1,000 patient days
How many patient falls result in injuries?
Approximately 25% of hospitalized patient falls result in injuries and 2% result in fractures.4
How does your unit define and record falls?
To measure the success of your fall prevention measures, you need to agree on what constitutes a fall. One commonly accepted definition is "an unplanned descent to the floor with or without injury to the patient."5 Recording both total falls and falls with injuries allows you to see if your unit’s preventative measures are working, even if falls resulting in injury are less common.
"Near falls" such as when a nurse or other staff member eases a patient to the floor after their knees give out should also be recorded. As well as occasions when a patient rolls out of bed, even if they land on a fall mat.
Beyond tracking the number of falls, tracking the fall rate can also be helpful. The fall rate, the number of falls per 1,000 occupied bed days, helps account for differences in how full/empty the unit was during different months. Tracking repeat falls can also be helpful in case one faller is skewing your data.
The procedure of documenting these falls will depend on the process your hospital or facility has in place. But tracking falls is crucial - if you can’t measure it, you can’t improve it.
The Role of Nurses in Fall Prevention Programs
The role of nurses varies based on staffing configurations and management decisions, but generally the nursing role in fall prevention includes:
- Completing and documenting patient fall risk screening and assessment
- Documenting patient-specific fall prevention practices
- Monitoring the patient’s medical condition for any changes
- Reporting falls to the physician
- Obtaining medical orders from the physician as needed
- Supervising nursing aides
- Educating the patient and family on fall prevention
- Obtaining the supplies (cane, walker, bed alarm, etc.) need to prevent patient falls
Nursing aides also play a part in preventing patient falls including:
- Evaluating the patient’s environment for safety during patient care tasks
- Performing care plan tasks and reporting to nurse when tasks are complete
- Reporting any changes in a patient’s medical condition to a nurse
Follow The Nursing Process for Falls
Following the nursing process - assessment, diagnosis, planning, implementation, and evaluation - reduces your patient’s risk of falls. Following all of these steps ensures you complete a fall risk assessment and use your judgement to adequately plan for each patient’s individualized fall prevention plan. Working with a multidisciplinary team helps ensure all of your patients needs are met.
Patient Fall Risk Factors
Performing a fall assessment is a crucial part of preventing falls. Fall assessments are typically performed during patient admission, after a patient transfers to your unit, after a change in care level or patient status, and after a fall.
Some risk factors that may be part of your fall assessment include:
- Age
- Previous fall history
- Gait instability
- Urinary incontinence
- Medication
- Patient care equipment
- Altered mental status
- High risk assessment evaluated via ABCS injury risk assessment (age, bones, coagulation, surgery)
Learn more about fall prevention assessments.
Universal Fall Precautions
Universal fall precautions are safety measures taken to reduce the risk of falls for all of your patients, regardless of their risk assessment. To help prevent falls you might follow some of these precautions:
- Allow your patient to become familiarized with their hospital room because falls are more common in unfamiliar environments.
- Teach your patient how to use the call light and allow them to demonstrate how to use it. If your patient knows how to call for assistance, they will be less likely to get out of bed on their own and possibly fall.
- Keep the call light and your patient’s personal belongings within reach, so your patient doesn’t need to get up to reach them.
- Answer call lights promptly, so your patient doesn’t get impatient and try to ambulate on their own.
- Keep the floors clean and dry. Promptly clean up any spills.
- Also, keep the floors free of clutter to reduce your patient’s risk of tripping.
- Bright lighting and nightlights make it easier for your patients to see while walking.
- Non-slip footwear (shoes or socks) keep patients from slipping.
- Grab bars offer support in your patient’s room, bathroom, and hallway.
- Lower the hospital bed when your patient is resting, in case of falls, and raise the bed when transferring for easier transfers.
- Keep the brakes locked on hospital beds to keep them in place.
- And keep the brakes locked on patient wheelchairs when they are stationary.
- Follow safe patient handling guidelines to keep yourself and your patients safe.
- Follow other universal fall precautions in place at your facility.
Patient-Specific Fall Prevention Strategies
You should create a patient-specific plan tailored to your patient’s unique risk factors to prevent falls. The specific interventions will depend on the patient. See the checklist below for common fall risks and strategies on how to prevent them.
- My patient has fallen in the past.
-
Discuss the cause of the previous fall and how to prevent it from occurring again.
- Ensure your patient has access to mobility aids, if needed.
Make sure your patients are always wearing non-slip shoes or socks.
Use a gait belt to assist your patients during ambulation.
Ensure your patient goes to their scheduled physical therapy.
- Follow a toileting schedule.
Use incontinence briefs and draw sheets.
Round hourly (alternating with a nursing assistant, if needed).
- Be aware of the potential side effects of your patient’s medication and develop a plan.
- Don’t use side rails with this patient (they may fall trying to climb over them).
Use a bed or chair alarm for continuous monitoring.
Use a floor mat to prevent injuries from falls.
Round hourly (alternating with a nursing assistant, if needed).
- Other intervention
Make sure your patients know their specific fall prevention plan. For one easy way to communicate with your patients, check out this free fall prevention interventions poster you can laminate to use in patient rooms.
Protect Your Patients from Injuries if a Fall Occurs
While the overall goal is to prevent patient falls, sometimes they happen. Using a padded fall mat helps reduce the risk of injury if your patient rolls or falls out of bed; they also come in fall mats with AEGIS, an antimicrobial shield.
Depending on your hospital or facility's policies, you may be expected to intervene if you see a patient falling. Don’t try to catch the patient, you could be injured. Instead lower your patient to the floor following these steps.6
Disclaimer: Always review and follow your hospital policy regarding this specific skill.
- If your patient starts to fall, step behind the patient in a wide stance and take one step back.
- Grab the gait belt or hip area of the patient for support.
- Bend one leg and place it between your patient’s legs.
- Slide the patient down your leg, lowering yourself at the same time to prevent back injuries. Prioritize protecting your patient’s head.
- Assess the patient for injuries once they are on the floor, before moving them. Reassure your patient and call out for help if necessary.
- If your patient is unable to get up, use a mechanical lift to prevent injury.
- Follow your hospital’s policy on recording and reporting falls.
Learn More About Fall Prevention
Ready to find out more about preventing falls? Check out this fall prevention article for more information.
References
- Agency for Healthcare Research and Quality. (2019). Falls. U.S. Department of Healthcare Research and Quality. Retrieved fromhttps://bit.ly/2KuOCKY
- Cameron, E. J., Bowles, S. K., Marshall, E. G., & Andrew, M. K. (2018). Falls and long-term care: a report from the care by design observational cohort study. BMC family practice. Retrieved fromhttps://bit.ly/2TxJ7yg
- Agency for Healthcare Research and Quality. (2018). Preventing Falls in Hospitals. AHRQ. Retrieved from https://bit.ly/32IHRv3
- Bouldin, E. L., Andresen, E. M., Dunton, N. E., Simon, M., Waters, T. M., Liu, M., … Shorr, R. I. (2013). Falls among adult patients hospitalized in the United States: prevalence and trends. Journal of patient safety.https://bit.ly/2Z7kWro
- Lunsford, B. and Wilson, L.D. (2015). Assessing Your Patients’ Risk for Falling. Retrieved from https://bit.ly/2OKjsU9
- British Columbia Institute of Technology (BCIT). (n.d.). 3.8 Fall Prevention. Retrieved from https://bit.ly/2H8TvY6
Medical Disclaimer: The information provided on this site, including text, graphics, images and other material, are for informational purposes only and are not intended to substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other healthcare professional with any questions or concerns you may have regarding your condition.








 France
France Australia
Australia