Falls are one of the leading causes of injury, hospitalization, and functional decline among older adults and medically complex individuals across healthcare settings. In both institutional and home-based environments, clinicians are tasked with identifying interventions that reduce fall risk while supporting mobility and independence. This balance is important in rehabilitation and long-term care populations, where restriction of movement can contribute to deconditioning, reduced confidence, and further functional decline.
Fall risk is multifactorial and may be influenced by cognitive impairment, medication side effects, post-surgical weakness, impaired balance, environmental hazards, or changes in continence status. Because of this complexity, fall prevention strategies often require layered interventions that address both physical and behavioral risk factors.
Among the technologies incorporated into fall prevention programs are bed exit alarms, chair alarms, and motion-based monitoring systems. When used appropriately, these tools can support caregiver supervision without limiting patient activity or participation in mobility.
What Are Fall Prevention Alarms?
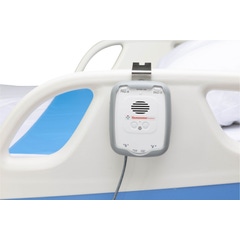
Fall prevention alarms are monitoring systems designed to notify caregivers when an individual initiates movement that may place them at risk for an unsupervised transfer. These devices are used when patients are identified as being at risk for attempting mobility without assistance.
Most alarm systems function through pressure-sensitive pads placed beneath a patient in a bed or chair, magnetic connections, infrared motion detection technology, or wireless monitoring platforms that detect weight displacement or movement from a support surface. When a change in position or pressure is detected, an audible or remote alert is activated to prompt caregiver response before an unsafe transfer occurs.
Monitoring systems of this type are used in acute care hospitals, skilled nursing facilities, assisted living environments, inpatient rehabilitation settings, and home-care environments where continuous supervision may not be possible.


Clinical Benefits of Alarm-Based Monitoring
When implemented as part of a fall prevention plan, fall prevention alarms may provide clinical benefits that support patient safety and caregiver response.
1. Early Caregiver Notification
Patients often attempt transfers in response to toileting needs, discomfort, confusion, environmental stimuli, or changes in cognitive status. In many cases, falls occur during the transition from sitting or lying to standing. Alarm systems allow staff or caregivers to respond at the initiation of movement rather than after a patient has already encountered a balance challenge or environmental hazard.
Notification may allow caregivers to assist with transfers, provide gait support, or redirect patients who are attempting mobility without supervision.
2. Support for High-Risk Populations
Alarm monitoring may be useful for individuals who demonstrate impaired safety awareness due to cognitive decline, delirium, or medication effects. Post-operative patients, individuals recovering from acute illness, and those experiencing medication-related sedation or orthostatic hypotension may benefit from monitoring during periods of elevated fall risk.
Patients with a history of falls or those undergoing functional decline during recovery may attempt independent mobility despite instruction to request assistance. In these situations, alarm systems can function as an adjunct to clinical supervision by supporting intervention when a patient attempts to mobilize without assistance.
3. Awareness of Movement Patterns
In some care environments, monitoring technologies may assist staff in identifying patterns of movement associated with increased fall risk. Repeated attempts to exit a bed during nighttime hours may indicate the need for scheduled toileting assistance or environmental modification.
When staff are trained in alarm placement and response protocols, monitoring systems may contribute to situational awareness and support fall prevention planning.
Appropriate Clinical Use Cases
Fall prevention alarms are not intended to function as standalone fall prevention strategies. Evidence supports their use as one component within a multifactorial fall prevention program that includes mobility assessment, environmental modification, and patient education.
Clinical scenarios in which alarm implementation may be appropriate include patients who attempt unsupervised transfers despite instruction, individuals with post-surgical functional limitations, those experiencing acute illness or medication changes, patients with impaired cognition or safety awareness, and individuals transitioning between levels of care.
Alarm use may also be appropriate in home-care environments when caregivers are present but unable to maintain observation. In these cases, monitoring systems can provide support by alerting caregivers when assistance is needed during transfers.
Alarm implementation should be individualized based on patient presentation, functional status, and supervision needs.
Integrating Alarm Technology into a Fall Prevention Strategy
The effectiveness of fall prevention alarms depends on patient selection, staff or caregiver training, and integration into a safety plan. Monitoring systems should be viewed as technologies that enhance supervision rather than replace clinical decision-making.
Outcomes are achieved when monitoring systems are combined with mobility assessment, transfer training, strength and balance interventions, medication review, environmental safety modifications, and scheduled assistance for activities such as toileting.
Fall prevention programs are most effective when they are proactive and multifactorial, requiring coordination between rehabilitation professionals, nursing staff, caregivers, and patients.
Supporting Safer Mobility with Sammons Preston®
Healthcare professionals and caregivers seeking fall prevention solutions may consider integrating monitoring technologies from Sammons Preston into fall prevention programming.
A range of bed and chair alarm systems designed for clinical and home environments is available through Performance Health and can be incorporated into safety planning.
New Sammons Preston Fall Prevention Alarms
References
- Mileski M, Topinka JB, Lee K, Brooks M, McNeil C, Jackson J. Alarming and alerting device effectiveness in reducing falls in long-term care facilities: a systematic review. Clin Interv Aging. 2019;14:2055-2065. doi:10.2147/CIA.S230334
- Subermaniam K, Wessels T, Wessels H. The effectiveness of a wireless modular bed absence sensor device for fall prevention. Front Public Health. 2017;4:292. doi:10.3389/fpubh.2016.00292
- Capezuti E, Brush BL, Lane S, Rabinowitz HU, Secic M. Bed-exit alarm effectiveness for fall prevention in nursing home residents: a randomized controlled trial. J Am Geriatr Soc. 2009;57(5):723-729. doi:10.1111/j.1532-5415.2009.02208.x
- Mileski M, Topinka JB, Brooks M, et al. Use of alarm devices to improve resident safety in fall-prone populations: a systematic review. Healthcare (Basel). 2019;7(3):91. doi:10.3390/healthcare7030091
- Shorr RI, Chandler AM, Mion LC, et al. Effects of an intervention to increase bed alarm use to prevent falls in hospitalized patients: a cluster randomized trial. Ann Intern Med. 2012;157(10):692-699. doi:10.7326/0003-4819-157-10-201211200-00005
- Dykes PC, Carroll DL, Hurley AC, et al. Fall prevention in acute care hospitals: a randomized trial. JAMA. 2010;304(17):1912-1918. doi:10.1001/jama.2010.1567
Medical Disclaimer: The information provided on this site, including text, graphics, images, and other material are for informational purposes only and are not intended to substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other healthcare professional with any questions or concerns you may have regarding your condition.








 France
France Australia
Australia